Long-Term Topical Steroid Effects: Withdrawal, Management & Recovery
By Dr. M. Khawar Nazir, MBBS, MSc Dermatology (Boston University, USA) – American Trained Dermatologist/ Skin Specialist in Lahore
A young mother in Lahore gently applies yet another layer of steroid cream to her toddler’s eczema, hoping for relief. After months of long-term topical steroid use, she notices the cream seems less effective and her child’s skin becomes fragile. When she finally stops the cream, the skin erupts in angry red patches and intense itching.
This heartbreaking scenario is a common story, highlighting the long-term topical steroid effects that can harm the skin and the daunting experience of topical steroid withdrawal. In this article, we delve into how prolonged use of topical corticosteroids can affect your skin, what withdrawal looks and feels like, and how to manage these effects with updated and evidence-based care.
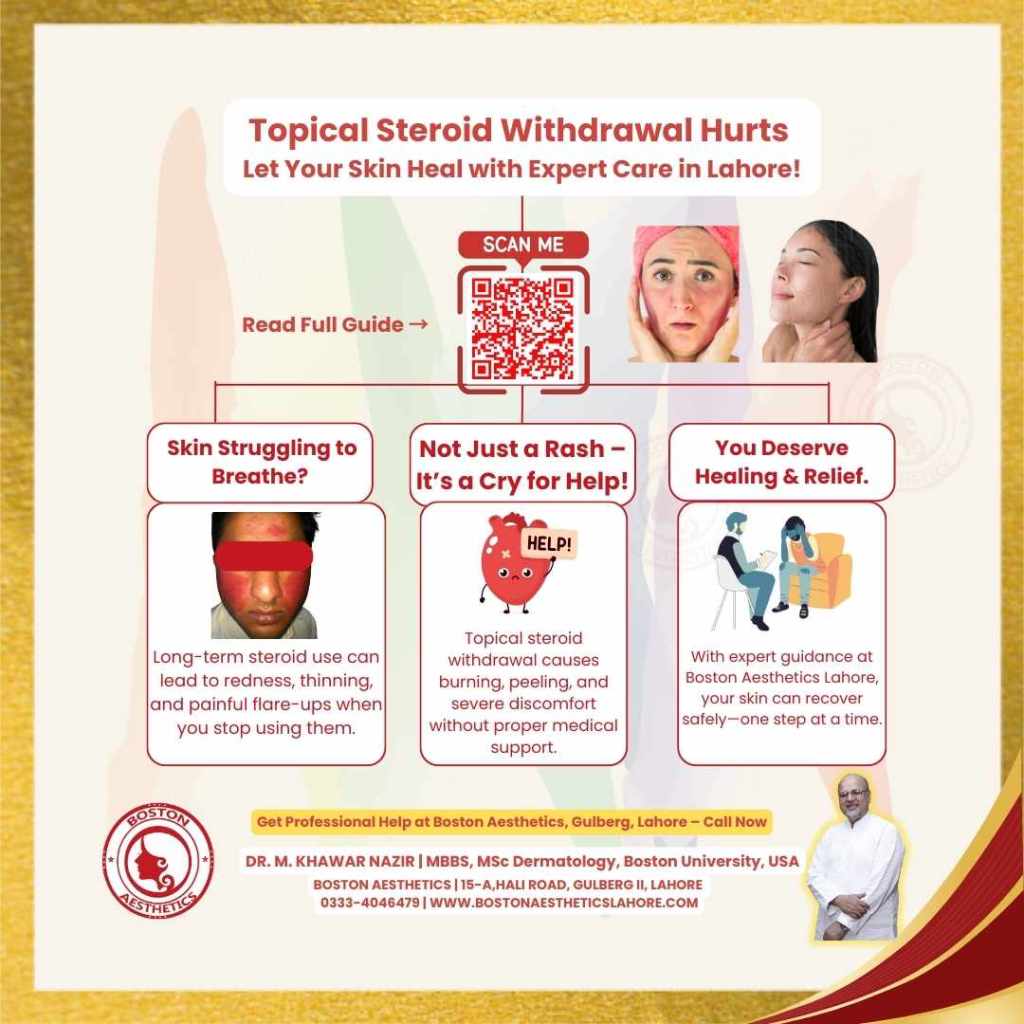
Table of Contents

Quick Overview: Topical Steroid Withdrawal – What You Must Know
1. What Is Topical Steroid Withdrawal?
A painful rebound reaction after stopping long-term steroid creams. It often causes burning, redness, peeling, and skin flare-ups worse than the original condition — physically and emotionally distressing.
2. Why Does It Happen?
Long-term use of potent topical steroids can make the skin dependent. When stopped suddenly, the skin struggles to adjust, leading to inflammation and discomfort. Misuse without a dermatologist’s guidance is a key cause.
3. Warning Signs to Watch For:
- Red, burning, or peeling skin
- Thin, shiny or fragile skin (skin atrophy)
- Intense itching or stinging
- Acne-like breakouts, pigmentation changes
- Emotional distress from chronic discomfort
4. How to Heal Topical Steroid Withdrawal Safely:
- Gradual tapering under expert care
- Use of gentle, supportive skincare
- Strict avoidance of self-medication
- Lifestyle changes and stress reduction
- Most importantly: expert medical supervision from a qualified dermatologist
5. Where to Get Help in Lahore:
At Boston Aesthetics, Gulberg, we offer compassionate, evidence-based treatment for steroid-damaged skin. Our American-trained dermatologist, Dr. M. Khawar Nazir, helps you safely recover, rebuild confidence, and reclaim your skin’s health.
🔔 Feel overwhelmed? You’re not alone. Healing is possible. Share this post to help someone suffering in silence.
Why Do People Use Topical Steroids Long-Term?
Topical steroids (also known as topical corticosteroids) are powerful anti-inflammatory creams and ointments that doctors prescribe for conditions like eczema, psoriasis, and severe allergic rashes. These medications can work wonders in the short term – reducing itch, redness, and swelling. In Pakistan, many individuals find steroid creams available at pharmacies even without a prescription. The warm, humid summers and dry winters of Lahore often trigger stubborn skin flare-ups, leading people to rely on these creams for extended periods. In some cases, people even misuse strong steroid creams as quick fixes for acne or to lighten their skin tone, influenced by cultural beauty standards. Initially, the steroid cream brings relief or a fairer complexion, creating an urge to keep using it.
However, using topical steroids beyond the recommended duration or without medical guidance can lead to dependency. The skin can become used to the steroid’s presence. Over time, higher strengths or more frequent application may be needed to get the same effect.
This cycle can silently turn into long-term use before one realizes it. In local dermatology clinics, it’s common to see patients who have unknowingly been applying a steroid cream on their face or body for months, even years. They often say, “It was the only thing that worked – until it stopped working.” This is a cautionary tale: while topical steroids are effective medicines, they must be used carefully and for limited periods as advised by a dermatologist to avoid serious side effects down the road.
Understanding Topical Corticosteroid Side Effects
Like all medications, topical corticosteroids have side effects, especially when used for a long time. The topical corticosteroid side effects on the skin can range from mild to severe. The most well-known issue is skin thinning from steroids. Doctors call this steroid-induced skin atrophy, which means the skin becomes thinner, delicate, and can bruise or tear easily. If you’ve ever noticed paper-thin skin or shiny, fragile patches after long-term steroid cream use, that’s atrophy.
But skin thinning isn’t the only problem. Prolonged steroid use can also cause:
- Stretch marks (striae): Reddish or purplish streaks can develop, especially where the skin is thin or where ointment was applied under occlusion (like covered with a bandage). Unfortunately, stretch marks from steroids are often permanent.
- Discoloration: Some areas might lose pigment and appear lighter (white patches), or conversely, some may develop darker spots. These changes can stand out more on brown skin tones common in Pakistan, causing distress.
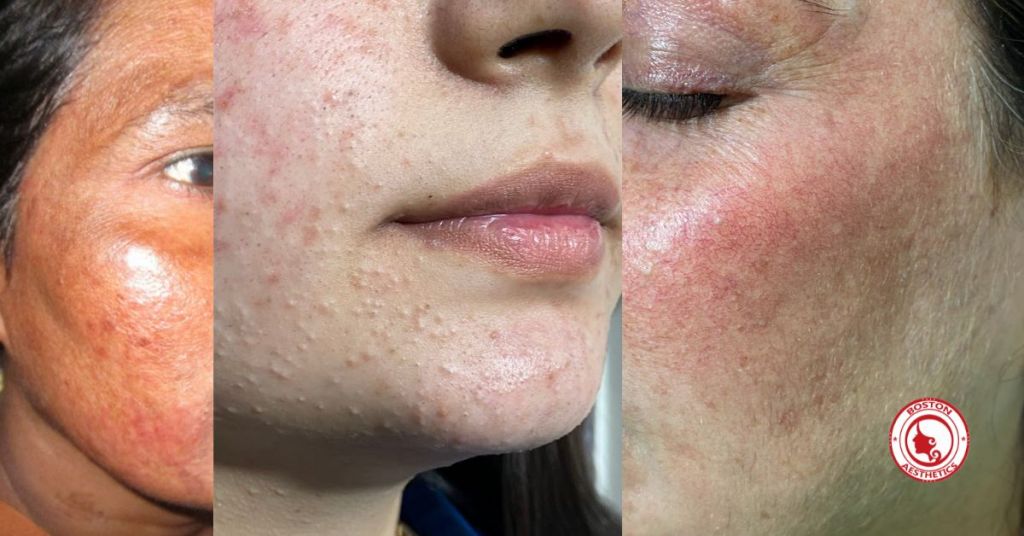
- Acne and bumps: Long-term use, especially of potent steroids on the face, can trigger acne breakouts or a rash around the mouth (perioral dermatitis) that looks like pimples. This often happens when people misuse steroid creams for cosmetic reasons.
- Visible blood vessels: You might see fine red blood vessels (called telangiectasia) appearing on the surface of the skin after chronic steroid use. This is due to the thinning skin and changes in blood circulation at the surface.
- Easy bruising and fragile skin: Even a slight scratch or bump can cause red or purple bruises (purpura) on skin that has been under steroid treatment for a long time.
- Infections: Steroids reduce local immunity in the skin. With long use, people can get more frequent skin infections – bacterial, fungal, or viral (like flare-ups of herpes cold sores) – because the body’s normal defense is weakened.
- Rosacea-like redness: Especially when strong steroids are used on the face, some develop a persistent redness and rash similar to rosacea. Paradoxically, stopping the cream can initially make this redness worse (a rebound effect).
- Tachyphylaxis: This is a medical term meaning the steroid stops working as well over time. The skin becomes tolerant to it, so the initial improvement fades even though you continue using the cream. This often tempts users to apply more frequent doses, further worsening side effects.
It’s important to understand that these side effects develop gradually. In many instances, the person using the steroid might not notice the subtle changes until the damage is significant. For example, a man applying a potent steroid on his feet daily for months might only realize his skin is paper-thin when he develops a painless cut that doesn’t heal easily. Or a young woman using a steroid-laden fairness cream might observe months later that her cheeks have fine red veins and breakouts that were never there before.
- Infographics in dermatology
- Patient Awareness Campaigns on Steroid-Induced Dermatitis | Boston Aesthetics Lahore
- 5 Proven Ways to Calm Mind & Glow Skin in Lahore
- 5 Steps to Confident Nose Reshaping in Lahore
- 5 Shocking Truths About Lip Laser Rejuvenation
Skin Thinning from Steroids (Steroid-Induced Skin Atrophy)
Let’s talk more about skin thinning from steroids, as it’s one of the hallmark long-term effects. Steroid-induced skin atrophy happens because these medications affect collagen, the protein that gives skin its strength and structure. With ongoing steroid use, the skin’s top layer (epidermis) and deeper layer (dermis) both become thinner verywellhealth.com.
You might notice the skin looks almost translucent, and veins that used to be hidden under the skin become visible. The skin may also develop a wrinkled, shiny texture in the area where the steroid was appliedverywellhealth.com.
If you pinch the skin of someone who has used steroids for a long time, it might feel delicate like tissue paper. Minor injuries can turn into larger tears. This thinning is often reversible to a degree: once the steroid is stopped, the skin can slowly rebuild thickness over a few months verywellhealth.com.
However, not everything returns to normal. If significant damage occurred, or if stretch marks formed, some changes can be lasting. That’s why recognizing and addressing steroid overuse early is so important.
The good news is that our skin is a living organ and has some capacity to heal. Dermatologists say that within about 1-2 months of stopping a topical steroid, you may see gradual improvement in skin thickness and strength. Supportive treatments, like gentle moisturizers or in-clinic procedures to stimulate collagen (for example, certain laser therapies or microneedling), may be offered to help restore the skin’s appearance. At Boston Aesthetics, Lahore, we utilize updated, evidence-based skin recovery services to aid patients dealing with steroid-damaged skin. This means each patient gets a custom plan, possibly including nourishing creams, vitamins for skin health, and advanced therapies, to maximize the skin’s recovery while ensuring no further harm.
What is Topical Steroid Withdrawal (TSW)?
When someone stops using a potent topical steroid after a long period, they may go through topical steroid withdrawal (often abbreviated as TSW). This condition is also known as Topical Steroid Addiction (TSA) or Red Skin Syndrome (RSS) in some cases. Essentially, the skin has become so used to the steroid that when the medication is removed, the skin “freaks out” because it has to adjust to life without the drug.
Imagine your skin as someone who has been on a long-term support (the steroid) and suddenly that support is taken away. The skin might rebound with intense inflammation. Instead of the original eczema or psoriasis you were treating, you get a severe reaction from the absence of steroids. Topical steroid withdrawal usually appears in the areas where the steroids were used most frequently.
Typical features of TSW include:
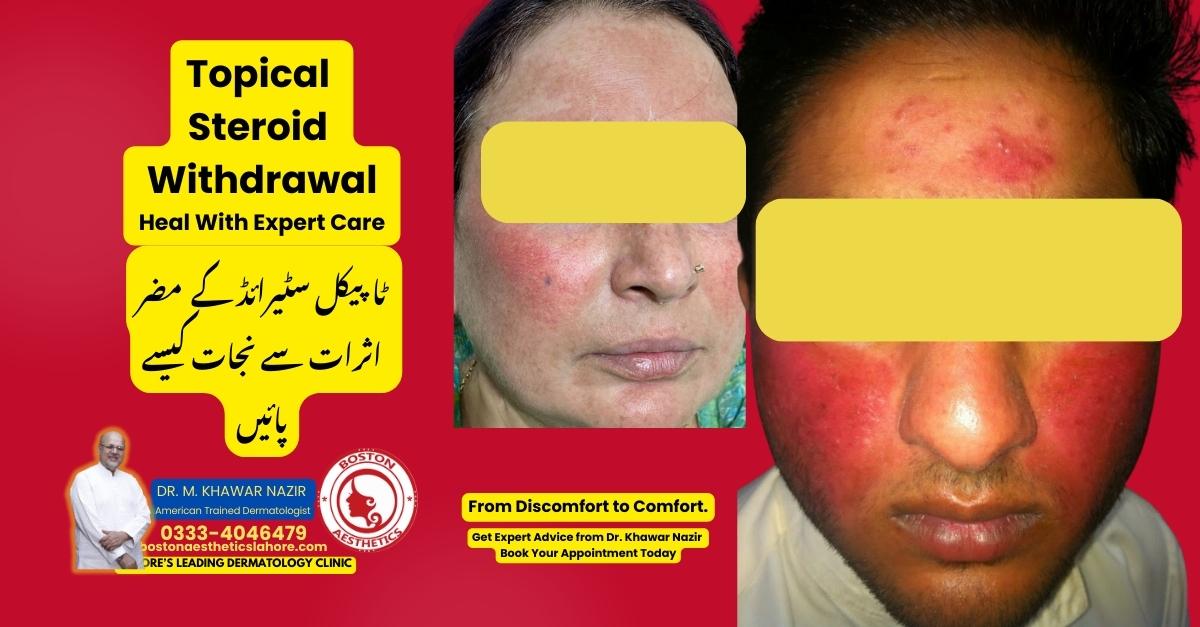
- Red, burning skin: People often describe it as feeling like a bad sunburn or as if the skin is on fire. The term “red skin syndrome” comes from this symptom – the skin can turn red, hot, and swollen.
- Intense itching: This itch is often much worse than the itch from the original eczema. It can be relentless and disturb sleep.
- Skin peeling and shedding: The affected areas may peel off or shed like after a sunburn. You might find flakes of skin on your clothes or bed.
- Oozing and weeping: Some severe cases have areas that ooze clear or yellowish fluid, as if the skin is crying. This fluid can dry and crust over, leading to cracks.
- Pain and sensitivity: The skin can be so raw that even soft clothing or a gentle touch hurts. Many patients say their skin feels sore all the time during withdrawal.
- Swelling: Especially on the face, you might see puffiness around the eyes or general swelling in the hands or feet if those were areas of steroid use.
- “Elephant skin”: In later stages of withdrawal, some people see a thickened, wrinkled appearance of skin in places, resembling the rough hide of an elephant. This is part of the cycle of the skin trying to heal and then flaring again.
- Emotional symptoms: The physical pain of TSW often comes with anxiety, depression, or a feeling of hopelessness. It’s emotionally exhausting to go through this ordeal.

Not everyone will have all these symptoms. The severity of topical steroid withdrawal can depend on how strong the steroid was, how long it was used, and individual factors like one’s skin and immune system. Generally, using a high-potency steroid daily for a year is more likely to cause withdrawal symptoms than using a mild steroid off and on for a few months. Women, especially middle-aged, seem to report TSW more often, but it can affect anyone – even children – who have had long-term steroid exposure.
One important point: TSW is not an infection and it’s not an allergic reaction to the steroid itself. It’s truly a rebound effect – the skin’s blood vessels and immune cells are reacting wildly after the calming influence of the steroid is gone. This means if you see a regular doctor who isn’t familiar with TSW, they might confuse it with uncontrolled eczema or another rash. That’s why awareness is key: if you suspect topical steroid withdrawal, you should consult a dermatologist experienced with this condition (like those at our clinic in Lahore) to get proper guidance.
Managing Topical Steroid Withdrawal and Healing Your Skin
Going through topical steroid withdrawal can feel like riding a physical and emotional roller coaster. There is no instant cure for TSW – and that’s a hard truth that doctors will gently share. However, there is hope and there are ways to manage the symptoms and support your skin as it heals. Here are some strategies and treatments for coping with TSW:
- Gradual tapering (if possible): If you haven’t stopped the steroid yet and are reading this in time, one approach doctors sometimes use is to slowly reduce the frequency or strength of the steroid instead of quitting abruptly. For example, if you were using a strong cream daily, they might switch you to a milder steroid or tell you to use it every other day, then less and less. This can sometimes soften the blow of withdrawal. Never just stop or taper without medical advice; always do this under a dermatologist’s guidance.
- Supportive skin care: Your skin barrier is extremely weak during withdrawal. Gentle care is crucial. Use plain, fragrance-free moisturizers liberally to combat dryness and help repair the skin barrier. Thick ointments like petroleum jelly or zinc oxide paste can protect raw areas. Taking cool or lukewarm baths with colloidal oatmeal or salt can soothe itching and reduce oozing. After bathing, pat the skin dry (don’t rub) and immediately apply moisturizer to lock in hydration.
- Medications for symptoms: While we avoid steroids during withdrawal (to allow the skin to recalibrate), other medications can help. Dermatologists in Lahore and worldwide might prescribe antibiotics if there are signs of infection (for example, if the oozing fluid turns yellow or if pain increases, which might indicate bacteria have invaded broken skin). Antihistamines (allergy medicines) can be given to reduce itching and improve sleep. In very severe cases, short-term use of systemic treatments (like immunosuppressant pills) might be considered to calm the skin, but this is decided case by case, weighing all risks and benefits.
- Alternatives to steroids: To manage the original condition (like eczema) during withdrawal, doctors may use non-steroid treatments. Calcineurin inhibitors (tacrolimus or pimecrolimus creams) are one option; they help control inflammation without steroids. Newer treatments for eczema, such as certain vitamin D creams or biologic injections (for severe cases), might be part of a comprehensive plan. The key is to control the skin condition so that you are not tempted to reach for steroids during the healing phase.
- Lifestyle and home remedies: Keep your surroundings cool, because heat can intensify the burning feeling. Use a humidifier in dry weather (Lahore’s winter air can be very arid) to prevent excess drying of your skin. Wear soft cotton clothing to avoid irritating your skin, and use mild detergents for laundry. Stress can worsen any skin condition, so finding ways to relax – gentle yoga, deep breathing exercises, prayer or meditation – can be helpful. Make sure to drink plenty of water and eat a balanced diet; some people find that anti-inflammatory foods (like fruits, vegetables, omega-3 rich nuts and fish) support overall skin health.
- Emotional support: Do not underestimate the emotional toll of TSW. People going through it have described feeling isolated and frustrated. Talk to friends or family about what you’re experiencing so they understand your struggles. Consider joining support groups (there are online communities for TSW; even if they’re not local to Pakistan, you can connect with others who understand). If anxiety or depression becomes overwhelming, consider speaking to a mental health professional. Remember, what you’re feeling is a valid response to a very real physical condition. Asking for help is not a weakness – it’s part of healing.
- Professional guidance and follow-up: Perhaps the most important management tip is to stay in touch with a dermatologist who understands TSW. Each person’s journey is a bit different. Regular check-ins allow the doctor to monitor your progress, adjust treatments, and ensure complications are caught early. At Boston Aesthetics in Gulberg, Lahore, we have helped many patients navigate topical steroid withdrawal with a structured program. We combine medical therapy with holistic care, guiding you week by week. Seeing improvement – even if slow – and having a professional reassure you can make a world of difference in staying the course.
- (no title)
- (no title)
- (no title)
- Acne and Scar Treatments
- Advanced Laser Hair Removal Lahore
- American Trained Dermatologist Lahore
- Anti-Aging Treatments by Dr. Khawar Nazir, Lahore
- Best Dermatologist in Lahore
- Best Hydrafacial in Gulberg Lahore
- Best Skin Specialist & Laser Clinic in Lahore
- Contact Us (Old Back up)
- Dermatologist in Lahore – Boston Aesthetics Gulberg II
- Expert Dermatology Services in Lahore | Boston Aesthetics
- Finding the Best Skin Specialist in Lahore
- Gallery
- Glow Facial in Lahore – Radiant Skin Awaits You!
- Hair Transplant Surgery in Lahore
- Home (Old Back up)
- Latest Skincare Trends by Dr. M. Khawar Nazir
- Medical & Advertising Disclaimer | Boston Aesthetics Lahore
- Medical-Grade HydraFacial Lahore | Book Now
- Men’s Grooming at Boston Aesthetics Lahore
- Patients Medical Record System
- Privacy Policy
- Skin Specialist & Laser Clinic Lahore
- Skin Specialist in Lahore
- Trusted Dermatologist & Skin Care Specialist in Lahore
- (no title)
- Experienced Dermatologist in Lahore
A Note on Time and Patience
One question we often hear is, “How long will this nightmare last?” The truth is, topical steroid withdrawal duration varies. Some people start seeing significant improvement in 3-4 months; for others, it might take over a year for their skin to substantially recover. It often depends on how long the steroids were used. As a rough guide, some dermatologists observe that the longer the steroid use, the longer the withdrawal period might be.
For example, someone who used a cream for 6 months might heal faster than someone who used one for 6 years. Many TSW sufferers report cycles of flare-ups and calm periods. You might have a few weeks where skin is calmer, followed by a flare of redness and itching, and this cycle can repeat. This is understandably exhausting, but over time, the flares tend to become less intense.
The good news is that withdrawal is a temporary phase, even if it feels endless while you’re in it. Your skin can and will heal given time and proper care. In our clinical experience in Lahore, we have seen patients who thought they would “never have normal skin again” make remarkable recoveries over months. Their skin gradually regained its natural color, the burning subsided, and they returned to living a normal life. Keeping that hope alive is important. Every week of progress, no matter how small, is a step toward recovery.
Preventing Long-Term Steroid Side Effects and Withdrawal
If you have a skin condition that sometimes needs topical steroids, you might be worried after reading about these issues. The goal of this information is not to scare you away from treatment, but to encourage safe use of steroid creams. When used correctly, under medical supervision, topical steroids can be a blessing for conditions like eczema by controlling flares quickly. Here are some tips to use topical corticosteroids safely and prevent long-term problems:
- Follow the dermatologist’s instructions: Always use the exact amount and duration prescribed. Dermatologists often recommend using strong steroids only for a short burst (like 1-2 weeks) and then taking a break.
- Use the right strength for the right area: Mild steroids (like hydrocortisone) are generally safer for delicate areas like the face or groin. Strong steroids (like clobetasol or betamethasone) are usually reserved for tough areas like thick psoriasis patches, and even then for limited times. Never put a super potent steroid on your face unless specifically directed by a doctor.
- Avoid using steroids as cosmetics: Do not use steroid creams to lighten your skin tone or as a routine face cream. In Pakistan, some beauty creams illegally include steroids and give quick brightening effects – avoid these at all costs. They can ruin your skin with long-term use. Always check if a cream contains a steroid (common names are hydrocortisone, betamethasone, clobetasol, mometasone, etc.) before using it for pigmentation or blemishes.
- Regular check-ups for chronic conditions: If you have a chronic disease like eczema that flares often, keep in touch with your dermatologist. Instead of constantly refilling an old steroid prescription, ask if there are steroid-sparing options. There are newer treatments and methods (like advanced moisturizers, medicated non-steroid creams, or even novel oral medications) that might control your condition and reduce the need for steroids.
- Listen to your skin: If you notice your skin getting thinner, developing odd red stretch marks, or that you need more and more of the cream to control your rash, pause and seek medical advice. These are red flags for overuse. It’s better to address it early than to wait until severe withdrawal forces the issue.
- Don’t abruptly stop long-term steroids on your own: If you’ve been using a strong steroid for a long time (several months or more), involve a dermatologist in the decision to stop. They can create a plan to taper it or replace it with something else. Stopping suddenly on your own could provoke a rebound (withdrawal) that is much worse than a careful, supervised discontinuation.
By taking these precautions, you can drastically cut down the risk of steroid-induced skin atrophy and other side effects. Remember, knowledge is power – understanding the proper way to use these medications means you get their benefits without paying a heavy price later. Educating patients in Lahore about these safe practices has become a mission for us, because we have seen firsthand how lives can be turned upside down by misuse. With the right approach, we can enjoy the relief steroids provide and avoid most of the pitfalls.
Frequently Asked Questions (FAQs)
1. What are the side effects of long-term topical steroids on skin?
Long-term use of topical steroids can cause skin thinning (atrophy), easy bruising, stretch marks, and changes in skin color. Your skin may become fragile, with visible blood vessels or acne-like bumps. These creams can also make skin infections more likely. Essentially, prolonged use can damage the skin’s normal texture and strength.
2. What is topical steroid withdrawal and why does it happen?
Topical steroid withdrawal (TSW) is a reaction that can occur after stopping a strong steroid cream used for a long time. The skin, which got used to the steroid, becomes red, itchy, and inflamed once the cream is stopped. It happens because the steroid was suppressing inflammation; when it’s gone, the skin rebounds with a severe flare as it readjusts.
3. How do I know if I’m experiencing topical steroid withdrawal?
If you quit a topical steroid and suddenly develop red, burning, itchy skin worse than your original condition, you might be experiencing TSW. Signs include redness in areas where the steroid was used, intense itching or burning, swelling, and peeling skin. It often feels like a bad sunburn or allergic reaction, but it’s actually the skin rebounding from losing the steroid’s effects.
4. How long does topical steroid withdrawal last?
It varies from person to person. Some people may go through withdrawal for a few months, while others might have symptoms for over a year. Generally, the longer you used a steroid, the longer the withdrawal can last. The symptoms do eventually improve, but it can take time (several months in many cases). Patience and supportive care are key during this period.
5. How can I treat topical steroid withdrawal symptoms at home?
You can manage many symptoms with gentle skin care and self-care. Keep your skin moisturized with plain, gentle creams. Use cool compresses or oatmeal baths to soothe burning and itching. Avoid hot showers and scratchy clothing that can irritate your skin. Over-the-counter antihistamines (allergy medicine) at night can help with itch and sleep. However, it’s important to also stay in touch with a doctor for guidance and to treat any infections or severe symptoms.
6. Is topical steroid withdrawal dangerous?
TSW can be very uncomfortable and even debilitating for a time, but it’s not typically life-threatening. The biggest concerns are severe pain, risk of skin infection due to open, cracked skin, and the emotional toll it takes. It’s important to have medical supervision during withdrawal to manage these risks. With proper care, people do recover from TSW safely, even though it feels extremely challenging in the moment.
7. Can skin thinning from steroid creams be reversed?
Skin thinning can improve after you stop using steroid creams, but it might take a few months. The skin slowly repairs itself and can regain thickness to an extent. If the thinning wasn’t too severe, it may almost return to normal. But some effects like stretch marks or very deep damage might be permanent. Dermatologists can suggest treatments like special creams or laser therapy to help improve thinned skin over time.
8. Are there safer alternatives to topical steroids for eczema and rashes?
Yes. For conditions like eczema, there are non-steroid creams (such as tacrolimus or pimecrolimus) that reduce inflammation without steroids. There are also new medicines, including biologic treatments for severe eczema, that can lower reliance on steroid creams. Using good moisturizers daily and avoiding triggers (like harsh soaps or allergens) can also help manage skin conditions with fewer steroids. Always discuss with a dermatologist to find the best and safest treatment plan for you.
9. How can I use topical steroids safely to avoid side effects?
To use topical steroids safely, follow the rule of “right medicine, right place, right time.”
Use the mildest effective steroid, only on the affected areas, and only for the time your doctor says (often no more than 1-2 weeks continuously).
Do not use steroid creams on sensitive areas like your face or genitals unless directed by a doctor, and never as a daily skin care product.
If your symptoms keep coming back, see a doctor again rather than just using the cream longer. Taking breaks and using other treatments (like moisturizers or medicated non-steroid creams) can reduce how much steroid you need.
10. When should I see a dermatologist about steroid side effects or withdrawal?
If you suspect you have side effects from a steroid cream – like unusual skin thinning, new stretch marks, or persistent redness – see a dermatologist as soon as possible. Early intervention can prevent further damage. Also, if you are trying to stop a long-term steroid and your skin is flaring badly, don’t suffer alone. Consult a dermatologist experienced in topical steroid withdrawal. In Lahore, you can reach out to expert skin specialists (for example, at Boston Aesthetics, Gulberg) who can guide you safely through the process and help your skin recover.
Conclusion
Long-term topical steroid use can feel like a double-edged sword: it brings relief at first, but may lead to fragile skin and topical steroid withdrawal that tests your strength and patience. If you or a loved one are facing the aftermath of heavy steroid cream use, know that you are not alone and there is a path forward. We have seen patients in Lahore and beyond regain healthy skin after going through this challenging journey. It takes time, proper care, and support, but recovery is absolutely possible.
The key points to remember are: use topical steroids wisely and cautiously, watch for early signs of side effects, and never hesitate to seek professional advice. If you are struggling with steroid side effects or withdrawal, reaching out to a dermatologist is not just advisable – it’s crucial. Expert guidance can ease your discomfort, prevent complications, and help restore your skin’s health sooner.
At Boston Aesthetics, Gulberg, Lahore, we offer updated, evidence-based skin recovery services for those dealing with steroid damage or withdrawal. Our approach is compassionate and personalized – we understand how deeply this issue can affect your life, and we’re here to help you heal, step by step.
Don’t let topical steroid withdrawal or side effects control your life. If you’re in Lahore or anywhere in Pakistan and need help, consult an expert dermatologist in Lahore today. The journey to healthy skin is easier when you have a caring professional by your side. Reach out to our team at Boston Aesthetics to start your healing process now – you deserve to feel comfortable in your own skin again.
Author: Dr. M. Khawar Nazir (MBBS, MSc Dermatology – Boston University, USA), American Trained Dermatologist/ Skin Specialist in Lahore.
Contact Information
Boston Aesthetics Lahore
15-A, Hali Road, Gulberg II, Lahore
For Aesthetic Treatments Appointment: 03334046479
Dr. M. Khawar Nazir, MBBS, MSc Dermatology, Boston University, USA
American Trained Dermatologist
Dermatologist, Cosmetic, LASER & Hair Transplant Surgeon
Also Available at Bahria Town Hospital
For consultations at Bahria International Hospital, Bahria Town Lahore, call at 042-111-296-297 for an appointment today.
If you can’t make it to the clinic, don’t worry—your skin health is still our priority. Dr. M. Khawar Nazir offers convenient online video consultations, allowing you to receive expert advice and personalised care from the comfort of your home. Whether you’re managing ongoing treatment or seeking advice on new concerns, our virtual consultations provide you with the same level of attention and care as an in-person visit. To book your online consultation, simply call or WhatsApp us at 03334046479.
Author Information:
Dr. M. Khawar Nazir, MBBS, MSc Dermatology, Boston University, USA
American Trained Dermatologist in Lahore
Dermatologist, Cosmetic, LASER & Hair Transplant Surgeon
Boston Aesthetics, 15-A, Hali Road, Gulberg II, Lahore | 03334046479
5 Steps to Confident Nose Reshaping in Lahore
Discover 5 simple, science‑based steps to achieve a confident, natural nose profile in Lahore using non‑surgical fillers. Safety meets elegance.
5 Shocking Truths About Lip Laser Rejuvenation
Discover the science, safety, and emotional impact behind fractional laser lip rejuvenation—designed especially for Asian skin types.
Does Sunblock Give Complete Sun Protection?
Sunblock helps protect skin but not 100%. Learn real sun safety tips from Boston Aesthetics Lahore.
Disclaimer: This article is intended for informational purposes only and does not substitute professional medical advice. Every individual’s condition is unique. Always consult a qualified dermatologist for diagnosis and treatment of any skin condition. Do not start or stop medications without professional guidance.








Leave a Reply